Rainbow glare: symptoms, causes, treatment
Rainbow glare is a rare mild optical effect of Femto-LASIK surgery. This page is dedicated to its description, causes, and surgical correction.
The following video summarizes part of the content of this page :
What is rainbow glare?
Rainbow glare is a rare optical side effect of femtosecond LASIK. It was first described in 2008 by Krueger et al. It affects a very few proportions of the patients that benefit from femtosecond LASIK technology to become spectacle and contact lens independent.
Rainbow glare is usually transient but may take some months to disappear. In some rare cases, it leads to persistent and disturbing visual symptoms, on which this page will focus.
Femtosecond laser technology to create the corneal flap (which is specific to the LASIK technique) was introduced about 18 years ago. It has progressively replaced the conventional microkeratome (blade cut of the flap) in the hands of most high volume refractive surgeons.
Patients affected by rainbow glare describe seeing a spectrum of colored bands proceeding in rainbow-like fashion. The effect is most prominent in the dark when looking at pinpoint light sources, such as oncoming automobile headlights at night.
When looking at monochromatic sources (for example a green neon or traffic light), lateral and vertical “ghosts” or replications or the source can be perceived.

Some of the patients have drawn with pencils or image softwares their subjective visual perception.
Typically, each radiating band contains a typical rainbow-spectrum color pattern, extending from violet– blue, to red at its outermost extent. In addition, some patients report a slight blurring of their vision.
The typical halos that may be reported after laser refractive surgery are different from the rainbow glare related visual symptoms. Typical halos look like a “spread” of the light emanating from the source, without any free interval. There are no distinct clear color fringes, although some slight colored scintillation may be observed at the edge of the halo or light streaks zone.
In rainbow glare cases, patients describe sharp colored radiating symmetrical halos extending laterally and vertically around bright light sources, from which they are separated by a free interval. These disturbances are usually seen with one eye only: in most of the reported cases, rainbow glare is unilateral or much more pronounced in one eye than in the other one.
The greatest perceived spectral intensity is noted when bright white light sources are visualized against a dark or uniform background. At day time, rainbow glare may not be perceived.
Typically, each radiating band contains a typical rainbow-spectrum color pattern, extending from violet– blue, to red at its outermost extent. In addition, some patients report a slight blurring of their vision.
What causes Rainbow Glare?
The cause of the rainbow glare was initially thought to be the diffraction of light from the grating pattern created either in the stroma or on the back surface of the LASIK flap after femtosecond laser use. Interestingly, rainbow glare may be the only medical and ophthalmic syndrome which is specifically caused by a pure diffractive mechanism.
The femtosecond laser spots are delivered in a raster pattern and are spaced very evenly. This is indeed the very even spacing of the spacing which causes the incoming light to diffract.
Diffraction is typically involved to explain the bending of light around the edges of an obstacle. In classical physics, the diffraction phenomenon is described as the interference of waves. Diffraction is very wavelength dependent; it occurs whenever light encounters « something » (particles, grating, striaes, slits etc.) which has a repetitive motive and dimensions close to the dimension of light waves (microns). The pattern of incoming monochromatic light after it has been diffracted by a small hole is the classic « Airy disc » (the smaller the hole, the larger the disc). The famous Young double-slit experiment, in which light is split into separate waves with various phase shifts creates a typical interference pattern.
Eventually, diffraction phenomena and lightwave properties are also « used » to conceive diffractive intraocular lenses, on which some little steps of a few microns can provide the separation of the incoming light in various foci.
In rainbow glare, light is diffracted by each of the impact zones. These zones represent a pattern of repeated and evenly spaced « optical disturbances », where the stromal tissue exhibits some different optical properties than the surrounding un-impacted zone.
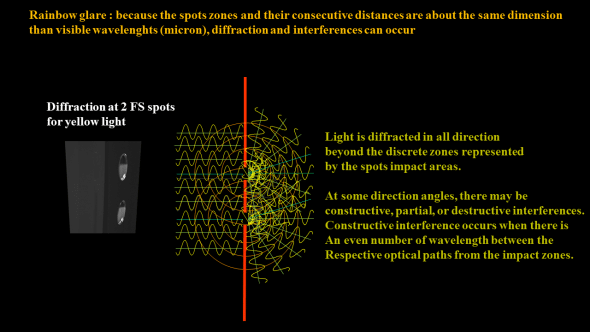
Each spot zone diffracts light and acts as if it was a « discrete » light emitter, spreading light in all directions beyond.
Given the particular geometry (again, the even distribution of the laser spots and the fixed dimension of the visible light waves), the following constructive interference phenomena will occur all the way along the direction of the laser raster spot lines in the corneal stroma. The following illustration limits this constructive interference phenomena to two adjacent spots:
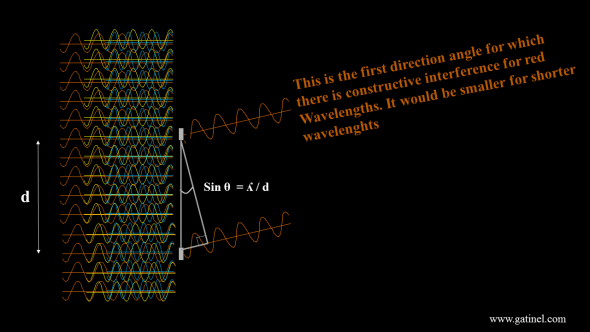
At some specific angle, which values depends on the spots spacing and considered wavelength, constructive interference will occur. Destructive interference (phase shift of half a wavelength) occurs for half the value of that angle.
Given the geometrical relationships between the light waves and the FS laser raster pattern, constructive and destructive interference will form at a specific angle, which will vary with the considered wavelength.
White light comprises a mixture of the wavelength present in the visible spectrum. Diffraction at the spots causes different wavelengths to separate. Because of this mechanism, which arises at the spots impacts plane, there is an obvious relation between the spatial distribution of the spots and the perceived diffraction pattern, which will be detailed later.
Rainbow glare has been initially reported after femtosecond LASIK using Intralase IFS 15 and 60 kHz (Abbot Medical Optics). We have reported the first case of rainbow glare consecutive to Femto-LASIK with a new-generation femtosecond laser FS 200 (Alcon Laboratories Inc).
The quality of the focused beam and numerical aperture of the focusing optics has been invoked to be the most significant factor in minimizing the diffractive dispersion of light that leads to this symptom. It is however intriguing that the occurrence of the rainbow glare symptoms is commonly unilateral, despite identical energy and spot separation parameters for the right and left eyes. In the clinical cases that we could analyze, the images taken by the Femto-laser camera after the flap creation were suggestive of an accentuated raster pattern for the shot delivery in the involved eyes, whereas it was not apparent in the contralateral eyes. How this immediate appearance after the interface creation relates to the occurrence and persistence of the symptoms remains to be elucidated.
Whereas the risk factors of rainbow glare remain obscure, the presence of hyper-reflective shot pattern with confocal microscopy examination reinforces the hypothesis that the uniform array of periodically aligned photodisruption defects acts as a likely source of the grating pattern, resulting in diffractive light scatter.
In Femto-LASIK surgery, the flap is lifted after being cut by the femtosecond laser, and the correction is delivered using the excimer laser on the exposed stromal surface. The correction of the refractive error incurs the etching of some stromal tissue (a lenticule of tissue is photoablated). On the other hand, the back surface of the reclined flap is not exposed to the excimer laser.

The excimer laser spots probably smooth out the raster pattern of the FS spots at the plane of the stromal surface of the cornea. However, the FS laser spots imprint could persist on the back surface of the LASIK flap.
Hence, it is believed that rainbow glare is caused by the grating pattern created on the back surface of the LASIK flap by the femtosecond laser exposure.
More on diffraction and rainbow glare
A diffraction grating represents an optical component with a periodic structure, which splits light into several beams with a specific direction. The directions of these beams depend on the spacing of the grating and the wavelength of the light.
The grating acts as the dispersive element. In rainbow glare, the incident light is refracted and diffracted by the back surface of the flap (within the corneal wall when the flap is in place) on his way from its source to the retina. The gratings created by the very evenly distributed femtosecond laser spots are of ‘transmission’ type. The diffracted light is composed of the sum of interfering wave components. The wave components depend in turn from the spectral composition of the light source. The intensity of the pattern created on the retina is the result of the combined effects of interference and diffraction.
It is common to assign a number to the principal diffracted beams of light, which are also called “modes”.
A diffraction grating has a ‘zero-order mode’ (where m=0), in which there is no apparent diffraction: a ray of light behaves according to the laws of refraction. The relationship between the grating spacing and the angles of the incident and diffracted beams (non-zero-order modes, m ≥1) of light is known as the grating equation.
When light is normally incident on the grating, the diffracted light will have maxima at angles θm given by this equation: d sinθm / λ = |m| where θm is the angle between the diffracted ray and the grating’s normal vector, d is the distance from the center of one slit to the center of the adjacent slit, and m is an integer representing the propagation-mode of interest.
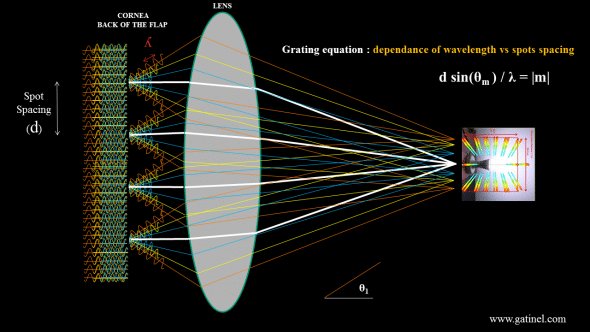
Schematic depiction of the rainbow glare global mechanism, for the 1st order of diffraction of incoming white light, which accounts for the « first » lateral band of rainbow glare. Similar constructive interference may occur at a larger angle (2nd order of diffraction). The « zeroth » order of diffraction receives the most energy, and correspond to none deviated (just diffracted light). Because this light does not deviate, it remains spectrally homogeneous and « white ».
The grating equation is useful to predict the location of the perceived color fringes, and their distance to the light source. Looking at a white-light source positioned at a distance of 1 m in a dark environment, the spectral bands for red extended from an apparent distance of about 10 cm for grating pattern spacing of about 8 microns.
Holding it’s smartphone flashlight at arms distance, one symptomatic patient pictured what is perception was:
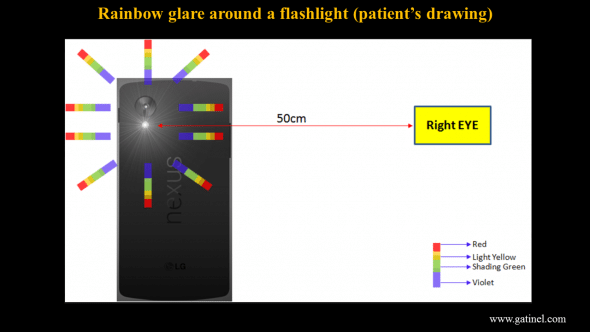
Patient’s representation of its rainbow glare when looking at a bright light source (smartphone flashlamp).
Simulation of rainbow glare
A transparent plastic calibration disc can be used to receive the pattern of a 9 mm diameter flap cut. We used the Wavelight FS200 femtosecond laser, and an 8×8 micron line/spot separation (the energy of the spots were slightly increased to take into account the rigidity of the plastic material).
This transparent disc bearing the raster pattern can be placed against the objective of a smartphone camera. The incoming light captured by the smartphone camera is diffracted at the plane of the spot impacts within the plastic disc, which is interposed between the light source and the smartphone’s objective.
This experience helps to visualize the dramatic effect of the light diffraction occurring in rainbow glare complicated LASIK cases.

Pictures taken through the FS treated plastic disc in Paris at night time. The rainbow glare patterns are particularly pronounced around the cars front lights.
On dimmer or less poly-chromatic lightings, rainbow glare can still be causing disturbing visual symptoms, such as the ghosting of bright traffic or pedestrian signs. Note that the vertical ghosts are sharper and brighter than the lateral ones (read further down for explanation).
Understanding the cause of the vertical extent of rainbow glare
A question must arise in one who understands the mechanisms of the diffraction attributed, in the case of rainbow glare after Femto-LASIK, to the regularity of the horizontal spacing of the spots.
If we understand that the regular spacing between the spots creates diffraction naturally oriented in the axis of the spots, it can be disconcerting that it is the vertical lines, perpendicular to the spot lines, which are perceived as the brightest of all!
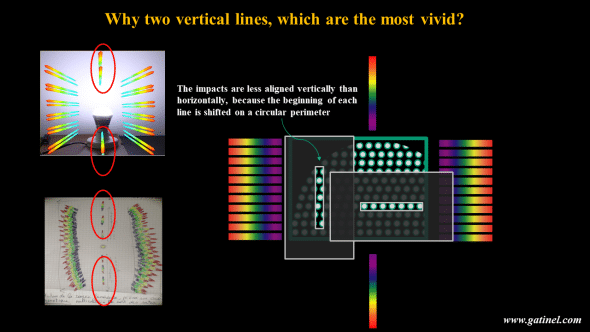
As the impacts are less aligned vertically, because of the line-wrap on a circular perimeter, there should be less constructive interference phenomena in the vertical direction. This is not the case clinically as patients report these vertical lines to be the brightest and the last to disappear over time
This phenomenon is created by the lines created by the parallel spots that diffract the light in the mutually perpendicular direction, like so many thin slits!
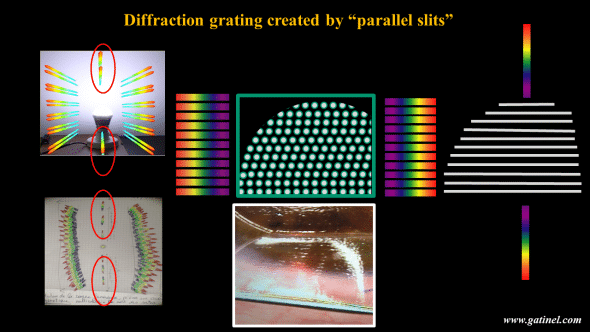
The explanation lies precisely in the fact that the parallel spot lines constitute fine lines for the incident light, which is diffracted in the opposite direction, and constructively. This back flap stromal pattern creates a diffraction grating produced by a large collection of evenly spaced parallel slits that produces a sharp interference pattern (1st order of diffraction) seen as a linear rainbow above and below a bright punctual light source.
Can rainbow glare be treated?
In most cases, rainbow glare vanishes within weeks or months after the LASIK surgery. In very rare cases, it may persist and cause the patients to stop driving at night, or develop anxiety. It is important for the clinician to make a proper diagnostic. I have met a patient who was sent 2 weeks in a psychiatric hospital since the verbal depiction of his symptoms led the unaware ophthalmologists (and later his shrine) to conclude that he was suffering from spectacular visual hallucinations!
We had reported the presence of a visible raster pattern at the interface after femto-assisted LASIK flap creation, using confocal microscopy (hyper-reflective spots have also been observed after Femto-LASIK in asymptomatic eyes).
These features are attributed to the tissular response of the femtosecond laser impacts at the posterior side of the flap, and in each of the cases we could document, hyperreflective spots were visible using confocal microscopy at the interface level.
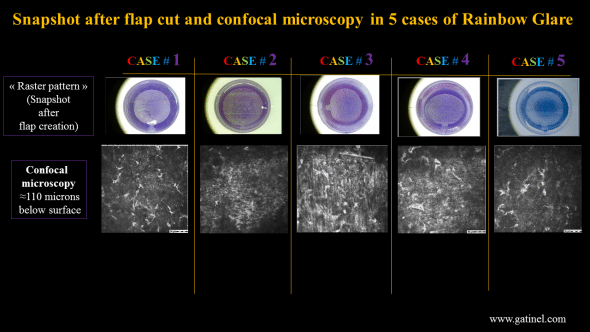
Images of the femtosecond laser flaps after their creation (top). Confocal microscopy at the flap interface, where the hyperreflective spots are clearly visible (presumably located at the back surface of the flap).
Erasing the evenly spaced singularities created by the impacts of the spots at the back surface of the flap seemed to be a logical and reasonable option to alleviate the patients with their persisting and debilitating symptoms. Undersurface ablation was described as an adjunct technique for LASIK enhancement in the case of too thin residual stromal bed, and we had experience with this technique in a reasonable amount of cases.
This validity of this hypothesis has been demonstrated by us since we have reported the first case of successful rainbow glare surgical correction using undersurface ablation of the flap for LASIK retreatment of low residual astigmatism. Since then, we have successfully treated two other cases of persisting and severe rainbow glare.
In the first performed case, confocal microscopy of the right and left corneas were obtained using the HRT II confocal microscope. On the right cornea, multiples rows of hyper-reflective spots appeared at about 125 microns below the anterior corneal surface. The horizontal and vertical distances between these zones matched the distance between spots and lines programmed in the FS200 laser (8μm).
At 6 months postoperatively, it was decided to attempt to correct the persistent residual astigmatism and rainbow glare symptoms by performing undersurface ablation of the LASIK flap.
A gentian violet pen was used to mark the center of the pupil on the cornea before flap lifting, and turning it back. The patient was asked to look down and the excimer laser delivered the astigmatism correction on the stromal portion of the flap.
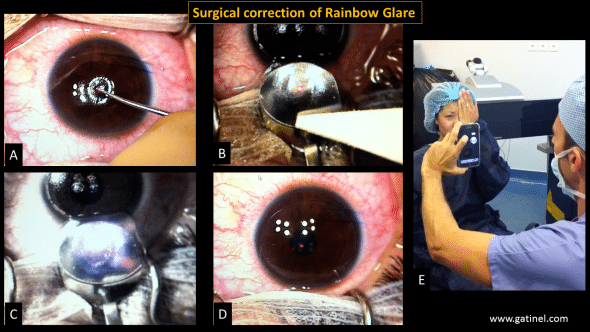
Legend: A: The right eye was draped in a sterile fashion, care was taken to keep the lashes out the surgical field. The peripheral cornea and the corneal center of the entrance pupil were marked with a blunt tip stained with a gentian violet solution. B While the patient was asked to look downward, the hinged anterior corneal flap was temporarily elevated and reclined on a flat domed spatula using a Merocel sponge. C The eye tracker of the EX500 excimer laser as deactivated, and the photoablation was delivered on the stromal bed, manually centered on the entrance pupil center mark. D the laser-treated corneal flap was replaced on the cornea, and the interface irrigated with a balanced saline solution before the flap was painted bath into position with a wet Merocel sponge. E: Before and after the completion of the procedure, the patient was asked to describe her visual perception by looking at a bright light white source. The typical rainbow glare pattern was present before the surgery but had disappeared immediately after.
Immediately after the procedure, a white flashlight was shone at 50 cm from the patient’s right eye. The rainbow glare pattern was no longer perceptible. At day one and day 30 controls, uncorrected visual acuity was 20/20 with the right eye, and the rainbow glare pattern perception did not reoccur. Based, on my experience, I would recommend a minimum of 15 to 20 microns for the depth of ablation (ex: PTK mode) for successfully erasing the raster pattern imprint on the back surface of the flap.
Recently, we have reported another case of successful backflap photoablation: undersurface photoablation which efficacy can objectively be followed by confocal microscopy, through progressively disappearing hyperreflective femtosecond laser impacts. This case shows that undersurface photoablation can be repeated if needed, although a single treatment would be preferred.
Conclusion
Rainbow glare is a post-LASIK optical side effect primarily caused by the diffraction of light. It is caused by the grating pattern created on the back surface of the LASIK flap after femtosecond laser exposure The diffracted light is composed of the sum of interfering wave components, and the intensity of the pattern created on the retina is the result of the combined effects of interference and diffraction. The risk factors for rainbow glare are not well understood.
Simultaneous correction of residual myopic astigmatism and rainbow glare proves that the grating pattern on the back surface of the LASIK flap causes rainbow glare. Our therapeutic success suggests that undersurface photoablation of the LASIK flap may be an effective method to reduce the symptoms related to rainbow glare. In eyes presenting with persistent and visually impairing rainbow glare symptoms, the deliverance of a planar ablation (e.g. phototherapeutic keratectomy) on the stromal side of the LASIK flap is also a valid option which we used in a further successful retreatment case.
References
- Krueger RR, Thornton IL, Xu M, Bor Z, van den Berg TJ. Rainbow glare as an optical side effect of IntraLASIK. Ophthalmology. 2008;115(7):1187-1195
- Bamba S, Rocha KM, Ramos-Esteban JC, Krueger RR. Incidence of rainbow glare after laser in situ keratomileusis flap creation with a 60 kHz femtosecond laser. J Cataract Refract Surg. 2009 ;35(6):1082-6
- Gatinel D, Saad A, Guilbert E, Rouger H. Unilateral rainbow glare after uncomplicated femto-LASIK using the FS-200 femtosecond laser. J Refract Surg. 2013;29(7):498-501.
- Maldonado MJ. Undersurface ablation of the flap for laser in situ keratomileusis retreatment. Ophthalmology. 2002;109(8):1453-64.
- Fernández-Vigo J, Macarro A, Fernández Sabugal J. Undersurface ablation of the corneal flap for LASIK enhancement]. Arch Soc Esp Oftalmol. 2007;82(11):697-703
- Taneri S, Azar DT. Ablation on the undersurface of a LASIK flap. Instrument and method for continuous eye tracking. Ophthalmologe. 2007;104(2):132-6
- Zhang Y, Chen YG. High incidence of rainbow glare after femtosecond laser assisted-LASIK using the upgraded FS200 femtosecond laser.BMC Ophthalmol. 2018 5;18(1):71
- Moshirfar M, Desautels JD, Quist TS, Skanchy DF, Williams MT, Wallace RT. Rainbow glare after laser-assisted in situ keratomileusis: a review of literature.Clin Ophthalmol. 2016 9;10:2245-2249.



Здравствуйте. Месяц назад сделала лазерную коррекцию методом фемто ласик. На правом глазу в ночное время беспокоят радужные эффекты от источников света ( слева и справа радужные полосы, причем их может быть по 2 на одинаковом расстоянии, а сверху радужные квадраты). Днём кстати тоже есть такая проблема, но это просто радужные пятна от источников света или отраженный свет, например в солнечный день о проезжающих машин. Так же болит глаз после того как посмотрю на яркие источники света , особенно белый и красный. Слева тоже заметила, но там в основном радужный квадрат над источником света в темноте. Так же на проблемный правый есть искажение цветовосприятия. Если посмотреть каждым глазом отдельно, то левым нормально, а правым ч виду в более теплых оттенках. Врач моя жмёт плечами и говорит, сто впервые такое слышит. Кстати , когда смотрю на телефон левым глазом вижу радугу на экране. Это может пройти или нет?
Hello! How can rainbow glare disappear? Does the pattern on the back surface of the flap erase itself?
Добрый день! Две недели назад сделали коррекцию зрения, от всех источников света и даже от солнца вижу исходящие радужные лучи, похожие на звезду но четко расположение по квадрату, также свет стал ночью намного ярче! Есть вероятность того, что это пройдет и через какое время, за две недели ничего не изменилось, у нас про такой случай слышат впервые, я даже не знаю как им объяснить что нужно сделать
В Украине открыто используют пациентов, не рассказывают про все возможные побочные эффекты, которые будут с пациентом до конца жизни после лазерной коррекции.
Мало того, лазерные хирурги специально умалчивают, а клиники специально создают определенные договора, чтобы снять с себя ответственность.
Лазерные хирурги просто зарабатывают деньги в первую очередь.
А все остальное не важно.
Это беспредел.
Если можно как-то повлиять на медицину, в частности, частную медицину в Украине – было бы прекрасно.
Мясники с медицинскими дипломами. Это кошмар 21 века.
The correction itself can be performed by any skilled refractive surgeon, but it requires a bit of experience (flap lift, eversion, delivery of a laser correction on the back flap surface..). This requires specific handling, and also some understanding of the rainbow glare mechanisms and means of correction.
Hello Dr Gatinel, I hope you are well. This article has been very valuable to me. Without being a specialist, I have been able to understand what happened to me during the Femtosecond surgery. I am from Colombia and I had surgery here 4 months ago and I see these patterns in the same way you describe. I consulted with the person who performed the surgery what occurred and did not receive a clear answer. I have a question: Understanding that my ophthalmologist did not correctly identify the rainbow effect, would he be able to correct me if it persists after 18 months? Or is it a more complex procedure that requires some experience?
It can take up to 18 months for rainbow glare to fully disappear. At that stage, if it persists, then it may not resolve completely.
Hlo Sir, Nitin again I am post-4.5 months from my lasik operation and my rainbow glare is fading away but at very slow rate. If it is fading away (even at slower rate) , Is there any hope that it wil fade away completely? I did my lasik on Alcon ex500 on 20th March 2023.
In reply to your message of 13 March:
Hello again. In my case, I also have HOA, but the main cause seems to be the flap’s decreased transparency., which reflects lights and produces severe glares and starburst-like lines from light sources day and night. This makes life very difficult. Can this strange flap problem also be solved by re-operation? (Have you had such an experience?) Or do I just have to wait for it to improve over time? I’m close to one-year post-op and still at a loss.
The diffractive process that generates the side horizontal rainbow glare is slightly different than that of the vertical brighter lines. The lateral diffraction is caused by the even spot separation along each of the femtosecond laser raster lines. The vertical bright line is caused by a line diffraction process; all the horizontal lines are involved (light diffracts perpendicularly hence the perceived direction) and all that light is concentrated in the vertical narrow band (whereas horizontally, a « spread » occurs). In most patients, rainbow glare disappear within 6 to 18 months postop.
Hlo Sir, my rainbow glare has reduced from horizontal sides but I am still seeing it brighter on vertical side. I had LASIK around 2 months ago. So, my question is that if it is reducing from horizontal sides then why is it not reducing from vertical side? Do you patients experienced completely diminishing of rainbow glare or they still see some of it.
Daytime symptoms are possibly due to interface problems, whilr halos at night can result from higher order aberrations. It is difficult to know precisely what explain your vision without direct examination and aberrometry measurements.
I had Lasik 10 months ago and I have daytime starburst and glare as well as common night ones. I believe this is caused by 1: Higher order aberrations caused by unnaturally flattened cornea 2: decreased transparency of the back of the flap and the corneal stromal bed due to scar tissue 3: uneven surface by an excimer laser
What do you reckon?
The visual disturbances have been tormenting me mentally and I’m desperately looking for a treatment with minimum damage to my corneal nerves. Do these laser treatments help improve my symptoms? I’m willing to do whatever it takes.
Cet effet est relativement rare mais pas exceptionnel. Le plus souvent transitoire; les raies colorées vont s’estomper progressivement dans les semaines à venir.
Bonjour,
J’ai des rainbow glare a J+1 de l’opération Lasik (fondation Rothschild justement) uniquement œil droit. Vision verticale d’arc en ciel sur lumière blanche. Je n’avais pas connaissance de cet effet secondaire. Est-ce vraiment transitoire ? À quel point est-ce rare ?
Merci
Rainbow glare refers more specifically to post FemtoLASIK unwanted diffraction effect. What you may see is different than the typical colored fringes; you may see radial/ starbust slightly colored images. This is usually caused by very small/microscopic structures that diffract light randomly. These structures may correspond to peculiar wound healing, local inflammation, etc.
I am experiencing rainbow glare and ghosting after PRK. It has now been over 6months since surgery and my consultant seems to have never really heard of this persisting and has no suggested remedy.
What are your thoughts?
If you wait some weeks or even months, you should see the vertical stripes of the side going away.. Usually, RG reduces and disappear over time. It can take up to 6 months to a year though.
Hi doctor,
I had lasik surgery 04 days ago on 06.10.22. since day 01 I am observing rainbow glare. It is observed in night only and outdoor only from distance more than 20 feet. As soon as I move further away rainbow on both sides of light also seems moving away. I can see green/yellow/red color on both sides of white object. Need guidance what is the reason and what should be management.
Hello Dr. Gatinel, thank you very much for your feedback and explanation. I assume you meant myopic rather than hyperopic astigmatism in this case? Since I have no issues at all with objects in close distance, only with light sources located further away (the ghosting symptoms disappear when I go closer towards the source).
If your ghost images are only located below the bright sources, it is probably not due to a diffractive mechanism such as in rainbow glare. RG causes image réplications that extend symmétrically around bright light sources and include all wavelengths. Here, what you could suffer from is residual more or less regular hyperopic astigmatism; it would be more apparent in the blue (short wavelength) because of the chromatic aberrations (increased refractive power in the blue vs. the red color range).
Hello Dr. Gatinel,
Since my LASIK surgery in 2020, I am suffering from « ghosts” (replications of the source) below green and especially blue monochromatic sources (for example a green traffic light) that are overlapping with the source image (like « shadows », no free interval). These « ghosts » are (almost) as bright as the source which often makes it impossible to identify the image from distance. The closer the object, the smaller the « shadows » get (seems like they « merge » into one image with the source when getting closer). The problem only exists with green and blue monochromatic sources, i.e., I do not see any colored bands in rainbow-like fashion when looking at poly-chromatic lightings. However, my surgeon assumes that the symptoms have the same cause as rainbow glare and could be corrected by undersurface ablation of the LASIK flap. Have you heard of these « partial » symptoms before?
Your symptoms probably relate to « ophthalmic migraine », which has little to do with the eyes; however, the visual aura usually concerns both eyes (it can be seen even if eyes are closed).
Salve Dott. Gatinel, ho fatto intervento Lasik per correggere ipermetropia e lieve astigmatismo, il 28 Dicembre 2021. Da subito dopo, ci ho visto bene da entrambi gli occhi, ho recuperato 10/10. Ma dall’ occhio sinistro, alle fonti luminose, vedo come se ci fosse un leggerissimo velo, che non rende perfettamente nitida l’immagine come dall’occhio destro. Ma quello che mi ha fatto impazzire è il fatto di vedere, ad esempio la sera, il lampione stradale illuminato, contornato da bande verticali con i colori dell’arcobaleno. Sui siti italiani, non c’è nulla che riporta informazioni relativo a questo fenomeno e tantomeno testimonianze. Ho avuto modo solo di poter conoscere una ragazza che come me ha lo stesso problema, dopo Lasik, ma ad entrambi gli occhi. A sua volta, è riuscita a tranquilizzarmi, perché ha conosciuto un signora, che ha vissuto la stessa esperienza e che ha affermato che è scomparso verso il 6° mese dall’intervento Lasik. Vorrei dunque sapere e magari avere conferma da lei e spero vivamente che sia così, che si tratti di un effetto transitorio, che, come ho letto qui, scompare tra i 6/9/12 mesi. L’idea di dovermi sottoporre ad altro intervento, mi terrorizza. Il mio oculista non mi è stato di grande conforto, forse non ha ben chiaro il sintomo descritto, ha detto in maniera molto fredda, che si tratta di un effetto collaterale, che era da mettere in preventivo, anche se non me ne aveva fatto parola e poi ha aggiunto che dovrei abituarmi ad un nuovo modo di vedere e li mi sono sentita morire! L’effetto che accuso io è minimizzato dal fatto che non lo vedo dall’altro occhio, per cui c’è una sorta di compensazione, e quindi non è debilitante, ma sicuramente fastidioso, di sera riuscirei comunque a guidare, se evito di centrare i fari delle auto che incrocio, con lo sguardo. Le chiedo quindi se, lei mi può dare quel conforto, che mi serve per affrontare il tempo di guarigione, con la giusta serenità. La ringrazio anticipatamente per la risposta, che vorrà fornirmi.
Hello,
My name is Florence from Uganda. I often get those flashlights and it normally affects one eye. I have experience this problem since 2014.
The light lasts for about 20 – 30 minutes. When the light disappears I get nausea and headache on both right and left side of the head. I have met eye specialists, I visited different eye clinics but they haven’t diagnosed any disease.
They always tell me that my eyes are working fine, my sight is very okay. And I have never had any surgery. My question is, what could be the possible cause? I need help. Thank you
Bonjour docteur
j’ai eu lasik sur
les deux yeux.
Suite à l’opération, j’ai des reflets arc-en-ciel sur les deux yeux. Mais vraiment invalidant sur l’oeil droit. Cela m’empêche de conduire la nuit et c’est vraiment handicapant pour mes études car la lumière dans la classe me fait avoir des arcs-en-ciel puis une migraine.
Plusieurs questions
Ils viennent de faire une retouche (il y a un mois), quand pourriez-vous intervenir pour corriger le Rainbow Flare ?
J’habite à Salt Lake City, mais je suis aussi français. Serait-il possible de
Quel est le prix de l’intervention ?
Avez-vous formé des médecins aux États-Unis pour cette procédure ?
Pouvez-vous expliquer la procédure à mon médecin?
Merci d’avance pour votre réponse, si vous souhaitez communiquer avec son médecin, merci de nous répondre en anglais.
Je pourrais également prendre un rendez-vous à distance si vous le jugez nécessaire.
Hi! Im an artist who actually had LASIK about 10 years ago and see 3 types of ocular halo/rainbows. I see one type of halo, mainly in my left eye, that I often attribute to a rise in blood pressure. I also see rainbow halos around lights and refracted light (starbursts which look like rainbow magnet fractals) around intense white light/sunlight. Because it’s been years and I learned how to oil paint after my surgery, I’ve been able to incorporate the rainbow light in much of my artwork.
I had/have pretty intense myopia (20/800+) and have long suspected I’m having asymptomatic migraines/seizures. I also have a few neurological abnormalities (type 1 narcolepsy, diagnosis of ASD as a child).
I’d encourage anyone seeing rainbows to refer the symptom as “seeing refracted light” – this helped lower some skeptical eyebrows for me.
I’d love to learn more about this symptom and I’d be happy to help in any way I can. Thank you for writing such an in depth explanation of what we may be experiencing.
I doubt that the rainbows that you perceive are exactly identical to those described by the patients operated with LASIK (very geometric and symmetrical colored sidebands). But it is possible that alterations in certain ocular tissues generate optical phenomena responsible for chromatic dispersion (often moderate despite everything). Corneal edema can induce a sensation of a colored halo. Only a well-conducted ophthalmologic examination can provide informed answers. Sometimes there are no obvious signs that could explain the visual symptoms experienced by patients.
Thank you for your comment. Could you send me a color illustration describing what you see around the lights? (gatinel@gmail.com). In general, the symptoms of RG, if it is indeed it, are transient, but the decrease can be slow, and spread over several months …
Hello Dr. Gatinel,
I had unsuccessful relex smile on right eye in December 2020 with visumax 500 laser. The cap and lenticule were misaligned, and I have a retained lenticule.
Since the second day, from my right eye, I see two concentric rainbow circles around spot sources of light with space in between (the second circle is much lighter than the first).
It seems there has been some fading, but it is hard to say, and I was hoping for more improvement by now.
Can you tell me based on your experience if there is any chance of full resolution with time, considering it’s already been 6 months without great improvement, if I have any options?
Thank you very much.
I am not sure, but one may try some glasses and hopefully, the filtration of some of the incoming light may improve the quality of vision.
Since PRK is performed without the need for a femtosecond laser (no flap cut) there is no chance of having rainbow glare symptoms per se. However, some color fringes can appear in some circumstances, due to various causes. Your surgeon should be able to provide you with relevant information about the optical zone centration and the quality of the correction.
Thank you so much for your answer and help Dr. Gatinel! Guess I’ll have to wait and avoid night driving for a little longer.
Do you recommend using any kind of glasses for rainbow glare (for night driving only)?
I saw some in Amazon but don’t know if they’re safe.
Thank you so much once again
Bonjour Dr Gatinel,
I have a sort of rainbow glare after PRK (moderate myopia, moderate astigmatism). Symptoms are rainblow colored starbursts/glare (day and night) from bright lights and triple images from monochromatic lights (rainbow spots from white lights) exactly like in the pedestrian sign image, except my ghost images are horizontal, not vertical. It’s been almost a year and daytime glare has become smaller, but at night it’s still very disturbing and the ghost images have not gone away. My doctor says my eyes look fine, no scars. Do you have any idea what could cause such rainbow glare after PRK? Will it diminish over time? I would really appreciate your insight since I can’t find any information about this side effect after PRK. Thank you!
Rainbow glare usually diminishes over time: the lateral bands become progressively fainter. The vertical colored spots usually persist longer. It can take about 6 to 12 months though. I would recommend that you wait at least one year before considering back flap surface ablation.
Hi, I did LASIK surgery 4 months ago, and I have rainbow glare since day 1 after surgery, didn’t fade away since. Is it possible it will fade away with time? I saw some studies where it says it’s even possible for it to go away after 18 months, do you confirm this or do you think it would be better to go for this photoablation surgery in the back of the flap? I have no reminiscent refractive error and I’m scared to go for another surgery just to fix it, but it bothers me so much, especially night driving. Hope you can help me, it’s been difficult months with little information, my surgeon knows nothing about it and just says it’s normal and will fade away with time, and there’s nothing to do it doesn’t.
Thanks for your message and consideration: before corrective surgery (back flap surface photoablation) is performed, a preoperative check is mandatory at the Noémie de Rothschild laser Institute in Paris. Getting appointments there online is possible via the website Doctolib (select Noémie de Rothschild laser institute as location). If the surgical indication is confirmed, then it can be performed in the coming days.
Hello,
I am located in Miami and just met with Dr. Florence Cabot the eye specialist at University of Miami Hospital Bascom Palmer location. I have been diagnosed with Rainbow Glare which I have been experiencing since August 2020 after I received Lasik procedure. Dr. Cabot recommended that I contact you. I hold a Irish passport and my family resides there still so I am thinking if I am to go ahead with corrective surgery I could possibly come to Paris? I need all the help and information that I can get. This has been a very scary and frustrating few months so I would be grateful if someone could help me please.
Très intéressant surtout avec une possibilité de réponse thérapeutique efficace :-)
Bravo encore et toujours ???