Position effective de l’implant
La position effective de l’implant est la position occupée par l’implant dans l’oeil après chirurgie de la cataracte. Elle affecte la valeur de la réfraction finale, car plus l’implant est « loin » de la cornée, et moins la puissance effective du couple cornée + cristallin est importante. De cette position, qui doit être anticipée (et repose alors sur une « assomption ») lors du calcul, dépend la puissance calculée pour l’implant (biométrie). Les formules modernes de calcul biométrique diffèrent principalement dans la manière dont elle « prédisent » la position effective de l’implant.
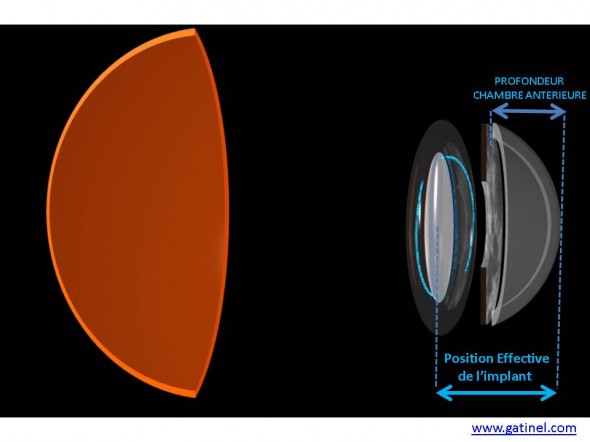
Représentation de la position effective de l’implant, qui est la distance entre le sommet de la cornée et le centre optique de l’implant (optiquement parlant, cette distance correspond à l’espace situé entre le plan principal image de la cornée et le plan principal objet de l’implant). Cette distance est différente (plus grande) de la profondeur anatomique de chambre antérieure. De plus, la profondeur de la chambre antérieure si mesurée en pré opératoire est modifiée par l’opération de la cataracte: l’implant étant moins volumineux que le cristallin, la chambre antérieure (anatomique) augmente après chirurgie de la cataracte.
Cette puissance d’implant, exprimée en dioptries (unité de la vergence : 22D par exemple) est destinée à donner à l’œil la réfraction souhaitée. Pour un même oeil (longueur axiale et kératométrie fixe) et une même réfraction visée, plus l’implant occupe une position proche de la cornée, et moins sa puissance est élevée. A l’inverse, si la position de l’implant est postérieure (plus loin du sommet de la cornée), alors sa puissance doit être plus élevée. Une différence de une à deux dioptries dans le plan de l’implant (soit 0.5 à 1. 5 D dans le plan d’une correction lunette) peut être obtenue en fonction de la position de l’implant.
Les illustration suivantes ont été réalisées grâce au biomètre IOL Master 700 (Zeiss):
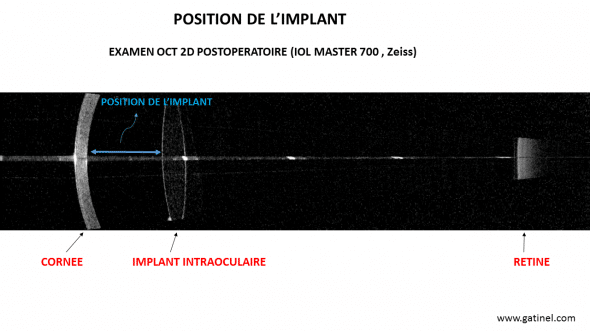
La position effective de l’implant n’est pas prévisible avant l’intervention. Cette image a été obtenue après implantation d’un implant de chambre postérieure au décours d’une chirurgie de la cataracte non compliquée.
Si un oeil est parfaitement emmétrope (pas de lunettes pour la vision de loin) après la chirurgie de la cataracte, c’est que le calcul d’implant a été effectué en prédisant une position de l’implant très proche de celle obtenue in fine, après l’intervention. Si l’implant occupe une position différente, une myopie (implant situé un peu plus en avant que prévu) ou une hypermétropie (implant situé un peu plus en arrière) seront observées.
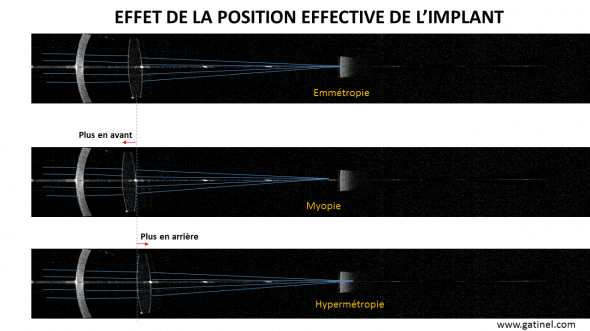
Représentation schématique des effets produits par le déplacement de l’implant vis à vis de sa position « attendue » (prédite par le calcul biométrique, en haut, pour une « emmétropie »).
Voici une liste non exhaustive des raisons qui expliquent l’impossibilité de prédire avec certitude la position de l’implant dans l’oeil après la chirurgie:
-le cristallin occupe un volume important: quand celui-ci est retiré, le volume du sac caspulaire est par définition réduit:
– le volume et la géométrie de l’implant diffère de celui du cristallin: l’implant est constitué d’une optique (6 mm de diamètre), supportée par des « pattes » (haptiques), qui peuvent être du même matériau que l’optique (implant dit monobloc) ou de composition différente (implant « 3 pièces » : une optique et deux haptiques).
– les implants diffèrent de part leur géométrie et leur position finale dans le sac capsulaire (dimensions de l’implant, angulation de l’optique vis à vis des haptiques de l’implant, etc.). La puissance focale de l’implant doit être mesurée depuis le plan principal image de celui-ci: la position de ce plan principal diffère selon l’indice de réfraction, l’épaisseur et la courbure des surfaces de l’implant.
– la profondeur anatomique préopératoire de la chambre antérieure est certes corrélée avec la profondeur anatomique post opératoire : mais cette corrélation est faible: par exemple, en cas de cataracte évoluée, la « protrusion » antérieure du cristallin réduit la profondeur de la chambre antérieure: celle-ci s’approfondit grandement après retrait du matériel cristallinien. L’épaisseur pré opératoire du cristallin joue également un rôle supposé dans la position finale de l’implant.
Voici une illustration de deux coupes de la chambre antérieure de l’oeil, effectuée par caméra Scheimpflug, avant et après chirurgie de la cataracte. On observe un approfondissement de la chambre antérieur de l’œil, lié en partie au retrait du volume du cristallin qui tend à faire « saillie » en avant de la pupille (le volume du cristallin augmente avec le temps).
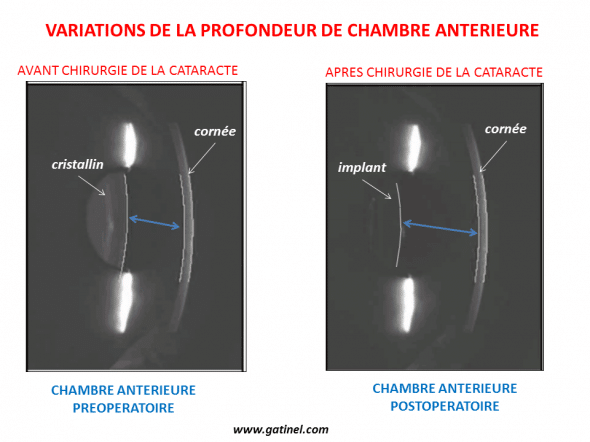
La chambre antérieure est plus profonde après le retrait du cristallin. Le volume de l’implant est nettement inférieur à celui du cristallin. La géométrie de l’implant diffère également de celle du cristallin : sa courbure antérieure est toujours moindre, car son indice de réfraction est plus élevé (Images avant et après intervention de cataracte, obtenues avec le biomètre AL-Scan, Nidek)
Les figures suivantes illustrent également ces données.
La première est une image acquise en coupe OCT du segment antérieur de l’oeil d’un patient atteint de cataracte bilatérale. L’oeil présente une hymermétropie, le cristallin est volumineux et repousse légèrement le plan de l’iris. La profondeur de la chambre antérieure préopératoire est réduite.
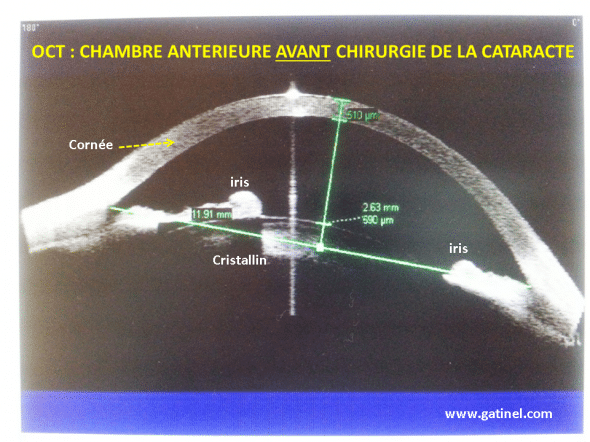
Avant l’intervention, le cristallin fait légèrement saillie dans la chambre antérieure (590 microns au centre en avant du plan de l’iris), ce qui réduit la profondeur de celle-ci (distance antre face avant de la cornée et face antérieure du cristallin : 2.63 mm)
Après retrait du cristallin (chirurgie de la cataracte par phaco émulsification) et pose de l’implant, l’OCT montre un approfondissement important de la chambre antérieure.
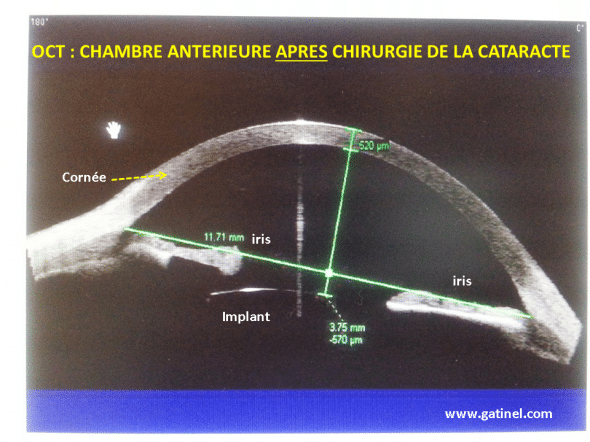
Après la chirurgie de la cataracte, qui consiste en le retrait du cristallin, et l’insertion d’un implant de cristallin artificiel, la chambre antérieure est approfondie. Cette modification est liée au retrait du volume occupé par le cristallin qui faisait « saillie » vers l’avant, en repoussant l’iris, et également au positionnement de l’implant dans le sac capsulaire: l’implant (face antérieure) est situé à environ 570 microns en arrière de l’iris. Il n’est pas possible de prédire avec certitude le positionnement de l’implant vis vis de la cornée, une fois injecté dans le sac capsulaire, après retrait du cristallin.
Il est donc important de bien comprendre ce point : la biométrie oculaire avec calcul d’implant comporte une part d’extrapolation : celle de la position finale (ou effective) de l’implant dans l’oeil.
Pour remédier à cette incertitude, les fabricants ont initialement proposé d’utiliser pour le calcul biométrique une valeur « moyenne », appelée « constante A », qui permet de réaliser le calcul biométrique en se fondant sur une position « moyenne » de l’implant dans l’oeil. Cette valeur était proposée après avoir accompli des études sur des yeux opérés de la cataracte et ayant reçu l’implant considéré. En fonction de l’écart entre les réfractions obtenues et souhaitées (erreur biométrique) il est possible statistiquement de trouver pour quelle valeur moyenne de position de l’implant l’erreur est minimale. Cette méthode nécessite que les autres sources d’erreur (mesure de la longueur axiale, estimation de la puissance cornéenne) soient le plus faible possible.
Position effective moyenne de l’implant
La position moyenne de l’implant est fournie par le fabricant, non directement mais sous la forme d’une constante exprimée en Dioptrie : cette « convention » est liée aux formules de calcul de première génération, notamment la formule dite « empirique » ou de « régression » appelée SRK (des initiales de ses auteurs). Cette formule est abandonnée, mais la formule SRK-T (T pour Théorique) est encore utilisée pour la plupart des yeux (à condition qu’ils ne soient pas trop « courts » – la longueur axiale doit être supérieur à 22 mm). La formule SRK-T fait partie des formules « théoriques », car elle repose sur un modèle physico mathématique de l’oeil. Cette constante est reliée à la distance entre le sommet cornéen et le plan optique (plans principaux) de l’implant: il ne faut pas la confondre avec la profondeur de chambre antérieure, qui est une donnée anatomique préopératoire (distance entre le sommet de la cornée et la partie antérieure du cristallin). Après l’intervention, la profondeur de la chambre antérieure peut être estimée en fonction de la distance entre le sommet de la cornée et le plan de l’iris. La position de l’optique de l’implant est différente de celle du plan de l’iris. Elle dépend de divers facteurs, comme la géométrie de l’implant, l’épaisseur de son optique, la géométrie du sac capsulaire (et de son insertion sur les procès ciliaires de l’oeil), etc. De plus, la technique chirurgicale utilisée est également à même d’influer légèrement sur cette position moyenne. Ainsi, la variable « position moyenne de l’implant » s’est vue substituer celle de « Surgeon factor (SF) » ou « Facteur lié au chirurgien » (formule de Holladay).
La constante A est exprimée en Dioptries: il est possible de la relier à la valeur de la position effective moyenne (PEM) de l’implant grâce à la formule suivante :
PEM = ( (constante A x 0.5663) – 65.6 +3.595 ) / 0.9704 )
La constante A est également convertible en « Surgeon Factor » (SF) :
SF = ( Constante A x 0.5663) – 65.6
La valeur de la constante A est généralement proche de 120 D. Dans la première formule, qui visent à convertir en « position moyenne » (mm), on observe que l’introduction d’une telle valeur (120) module la valeur de la PEM autour de 5 mm environ.
Dans la seconde formule, la valeur obtenue est plus faible: cette valeur est un « correctif » à appliquer à une constante représentant la position moyenne de l’implant.
Position effective individualisée de l’implant
L’individualisation de la position effective prédite de l’implant au moyen des données biométriques recueillies pour un oeil donné est au cœur des enjeux des formules modernes de calcul biométrique. Le premier auteur a avoir modifié intentionnellement la valeur de la constante A fut Binkhorst; il proposa d’augmenter la valeur de la position effective de l’implant proportionnellement à longueur axiale mesurée. La justesse de la prédiction de la position effective pour un oeil particulier détermine la qualité du résultat réfractif obtenu. Dans les yeux « atypiques », ou opérés dans le passé de chirurgie réfractive, les assomptions des formules de 1er, 2e et 3e génération (formules de calcul d’implant) se révèlent erronées. Les formules de 4e et 5e génération sont plus à même de réaliser un calcul plus précis.
L’influence de la position effective de l’implant est illustrée dans le calcul de la puissance de l’implant après chirurgie réfractive (LASIK pour myopie), chez un patient atteint de cataracte après qu’il eût été opéré de LASIK pour myopie dix ans auparavant.

Cataracte bilatérale survenue plusieurs années après réalisation d’un LASIK pour corriger la myopie (dossier de correction non disponible). L’instrument OQAS / HD ANALYZER révèle une élévation de l’indice de diffusion lumineuse (optical scatter index OSI), dont le seuil est généralement fixé à 1.5. La face antérieure de la cornée a une géométrie oblate.
Le calcul biométrique, destiné à fournir la puissance de l’iplant, peut être accompli en utilisant deux formules différentes. Ces calculs sont fondés sur les mêmes éléments (kératométrie, longueur axiale, et profondeur de la chambre antérieure pour la formule de Haigis). Ils fournissent cependant des résultats légèrement différents, car les formules prédisent une position effective de l’implant différente.
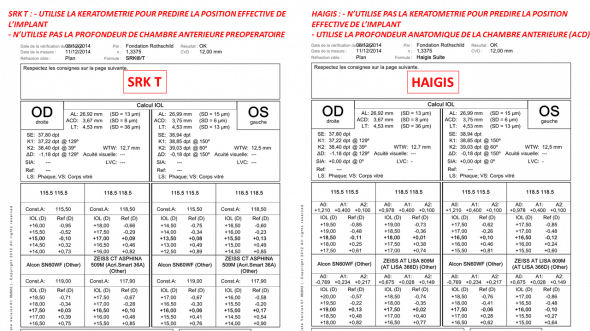
Pour une même réfraction cible, la formule SRK T prédit une puissance légèrement inférieure à celle de la formule de HAIGIS. Cette différence est spécifiquement induite par une prédiction de la position effective de l’implant qui n’est pas identique entre les deux formules. La formule SRK T ne tient pas compte de la profondeur de la chambre antérieure, et se fonde sur la kératométrie et la longueur axiale pour prédire la position de l’implant. La chirurgie par LASIK ayant modifié la kératométrie, l’utilisation de celle-ci pour prédire la position effective de l’implant devrait être caduque. Une kératométrie réduite (comme après LASIK myopique) prédit une distance entre cornée et implant plus faible qu’une kératométrie plus élevée. La formule de Haigis n’utilise pas la kératométrie pour la prédiction de la position de l’implant.
Légende : AL longueur axiale (myopie), ACD: profondeur de chambre antérieure anatomique préopératoire, LT: épaisseur du cristallin (lens thickness), SE: équivalent sphérique de la puissance cornéenne, K1 : K2 : kératométrie des méridiens le moins vs le plus cambré.

Laisser un commentaire